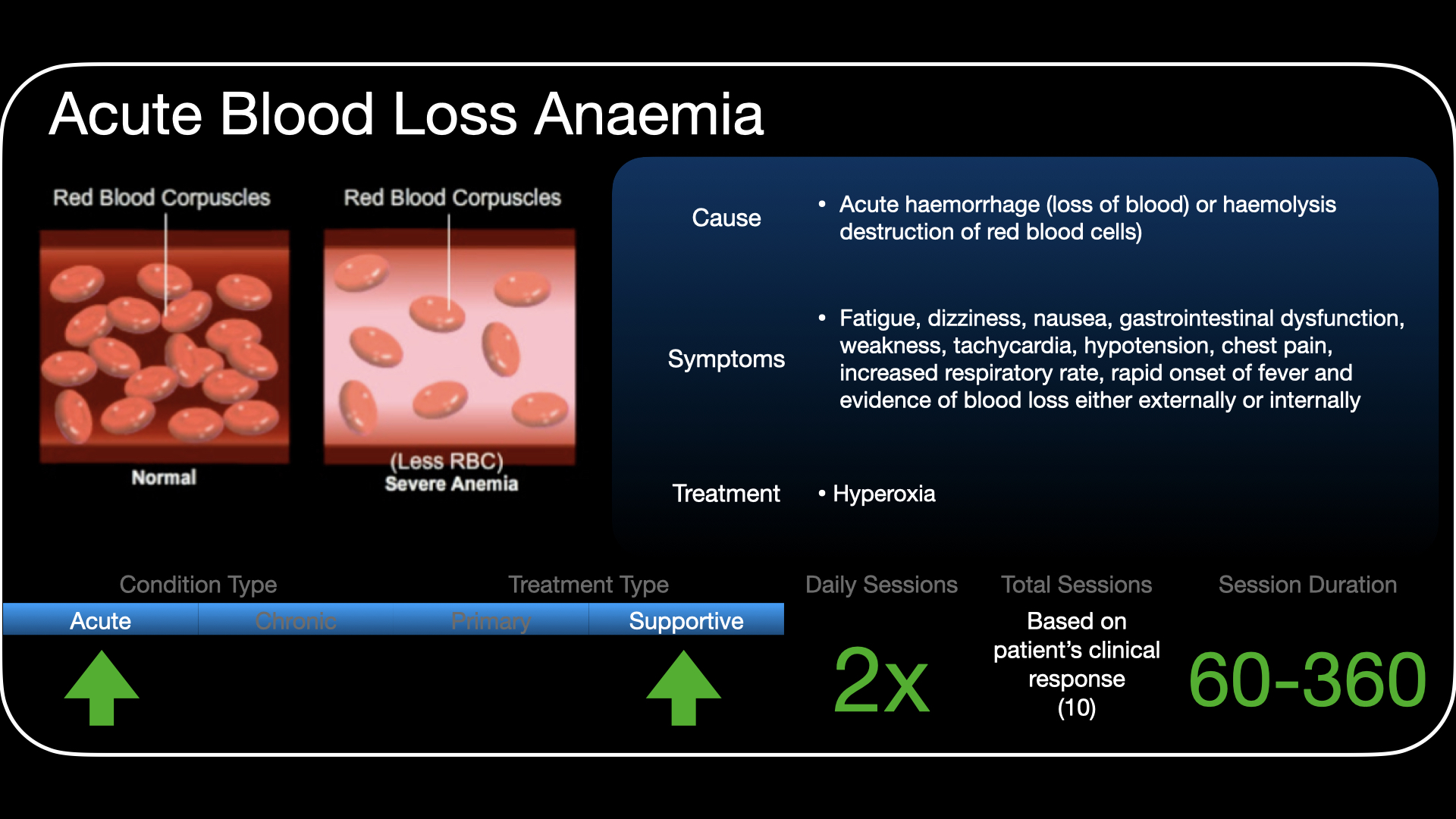
Severe Blood Loss Anaemia
Source: http://www.uhms.org/
Haemoglobin (Hb), a powerful carrier for oxygen, carries 1.38 ml of oxygen per gram. The amount of oxygen that will dissolve in one millilitre of plasma is 0.003 ml per mmHg of the partial pressure of oxygen (O2) in inhaled gas. CaO2 and CvO2 respectively represent the arterial or venous content of oxygen in blood. The formula for determination of arterial oxygen content is given as follows:
CaO2 = (grams Hb x 1.38 ml O2 x % O2 Hb) + (0.003 + O2 x mm pO2)
Oxygen delivery (DO2) is calculated by multiplying arterial O2 content by cardiac index: DO2 = CI x CaO2
(CI) and is given by the following formula: CI = cardiac output (CO) ÷ m2 body surface area (BSA)
Oxygen consumption (VO2) is calculated by the Fick equation given by the following formula:
VO2 = CO (CaO2 – CvO2)
On the average, the body extracts 5 to 6 ml of O2 for every 100 ml of blood that sweeps through the micro-vasculature of most organ systems. Physiologic normal levels of Hb readily supply tissue oxygen extraction rates of 5 to 6 volume percent. As Hb drops to 6 g/dl, oxygen delivery, to offset these baseline oxygen extraction rates, becomes problematic and is clearly inadequate at Hb levels below 3.6 g/dl.
Accumulative oxygen debt is defined as the time integral of the VO2 measured during and after shock insult minus the baseline VO2 required during the same time interval. Clinical research in evaluation of patients with severe haemorrhage, demonstrates no chance of survival if the accumulative oxygen debt exceeds 33 L/m2. Multi-organ failure (MOF) occurs if the accumulative oxygen debt exceeds 22 L/m2. All patients who have an accumulative oxygen debt of 9 L/m2 survive without residual disability.
Clinical Setting
Inability to transfuse red blood cells (RBCs) in severe anaemia occurs when the patient refuses blood upon religious grounds or if the patient cannot be crossmatched to receive blood. Transfusion-transmitted infection (TTI), while statistically now less likely with nucleic acid testing (NAT) [approaches 1 per 2,000,000 units transfused for both human immunodeficiency (HIV) and hepatitis C (HCV)], still prompts patients to exercise their right to refuse transfusion.
Untoward inflammatory and immuno-modulatory effects of large RBC transfusions may also be a reason to seek alternatives. Blood substitutes, by way of use of perfluorocarbons or cell wall free polymerised Hb are still undergoing randomised clinical trials. While both approaches demonstrate advantages as well as disadvantages, neither have yet had final FDA approval for routine clinical uses. Both approaches are still compatible with adjunctive hyperbaric oxygen (HBO2) therapy. HBO2 therapy for severe anaemia has had a long-standing approval for use by the Centres for Medicare and Medicaid Services (CMS) and its predecessor, the Healthcare Financing Administration (HCFA).
Pulsed HBO2 therapy provides a way to clinically rectify accumulating oxygen debt in severe anaemia when transfusion is not possible. The patient initially can be placed at treatment pressures of 2.0 to 3.0 ATA or 0.2 to 0.3 mPa (million pascals) of oxygen with air breaks for up to three or four hours with surface interval titrated to avert symptoms associated with reoccurring oxygen debt. Occurrence of end organ dysfunction (altered mental status, ischaemic EKG change, sprue-like diarrhoea from ischaemic bowel, hypotension, diminished urinary output, etc) also may be used as guidance, but are less desirable as their advent represents more progressed end points of illness or injury. By adjunctive use of haematinics, the surface intervals between HBO2 treatments can be lengthened gradually until the patient's baseline anaemia builds to allow for proper O2 delivery.
Role of Hyperbaric Oxygen Therapy
The two most prodigious oxygen using, mammalian organ systems are the heart and the brain. Oxygen extraction rates of these systems based on patient activity are 6 ml of O2 per 100 ml of circulated blood in the brain and 10-20 ml of O2 per 100 ml of circulated blood in the heart.
As early as 1959, Boerema demonstrated that swine which were exchanged transfused with 6% dextran/dextrose/Ringers' lactate solutions to produce Hb levels of 0.4 to 0.6 g/dL could survive in the short-term if they underwent assisted O2 ventilation in a hyperbaric chamber at 0.3 MPa. HBO2 therapy has repeatedly allowed survival in what would have otherwise clearly been unsurvivable clinical circumstance without blood transfusion.
HBO2 therapy provides a way in severe anaemia to successfully correct accumulating oxygen debt in untransfusible patients.
Evidence Based Evaluation of Hyperbaric Oxygen Therapy by the Undersea & Hyperbaric Medical Society's Hyperbaric Oxygen Committee Standard Approval Criteria
In medical resuscitative intervention, the American Heart Association (AHA) evidence based criteria is wisely accepted to guide clinical therapeutic intervention. Normobaric oxygen (NBO2) is considered a class I indication while HBO2 may be a class II.b. indication.
Rather consistently the body of literature confirms over and over again better survival in animal models of both haemorrhage to a predetermined mean arterial pressure (Wiggers model) or fixed volume haemorrhage. Both increased short-term and long-term survival for HBO2 groups over normobaric air (NBA) or NBO2 groups.
In summary, both by the support of animal work and human clinical experience evidence-based analysis firmly supports the use of HBO2 as a treatment option in severe anaemia using AHA, NCI-PDQ, and BMJ evidence-based criteria.
Gregory Weir Vascular Surgery
Vascular & Hyperbaric Unit
Life eugene Marais hospital
The purpose of this web site is to offer Dr Weir’s patients and their families access to information regarding hyperbaric oxygen therapy, wound care and vascular disease in general as well as specific information on certain disease processes. The information on this site does not necessarily apply to all patients with the same diagnosis. If you are not a patient of Dr Weir, please do not regard the information on this website as a substitute for a thorough assessment by a qualified Vascular Surgeon. If in doubt, consult your doctor.
